Use of HemaShock® in Shock
Pathophysiology of Severe Shock
Severe Hemodynamic Shock is characterized by poor tissue perfusion. This results in reduced organ (e.g. brain, heart, kidney, etc.) function and a switch to anaerobic metabolism, acid formation, and loss of arteriolar tone.
When this happens the arterioles and veins dilate and blood pools in the periphery, which further reduces blood pressure and cardiac output.
Types of Hemodynamic Shock
There are several categories of Shock
1. Hypovolemic shock where blood volume is lower than normal (blood loss, dehydration, diarrhea (cholera))
2. Distributive shock where the total volume of the circulation is larger than normal (septic, anaphylactic, neurogenic, toxic)
3. Pump failure shock where the heart fails to pump blood into the circulation (cardiogenic)
4. Obstructive shock where blood flow into the right or left ventricles is impeded (cardiac tamponade, pulmonary emboli, pneumothorax)
HemaShock® is indicated for use in severe shock of categories 1 and 2. It is not currently recommended for categories 3 and 4.
Treating Severe Shock with HemaShock®
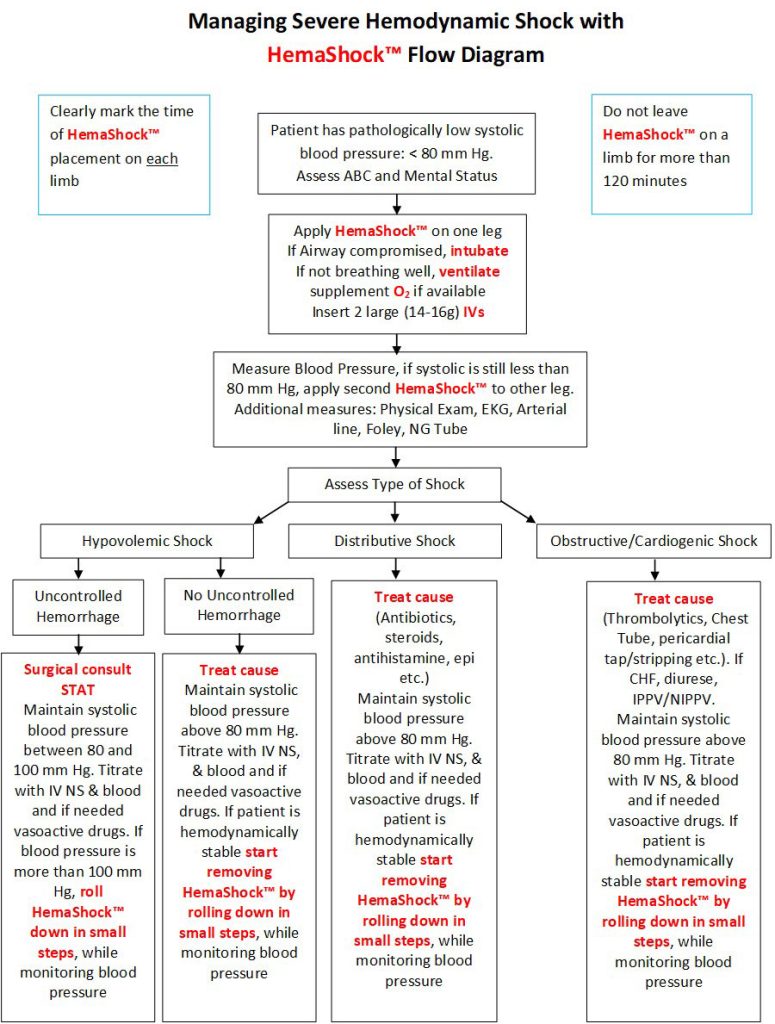
In addition to the standard treatment (fluids, blood, vasoactive drugs, supportive measures), apply HemaShock® to one leg and measure blood pressure. If the systolic blood pressure continues to be pathologically low (e.g. below 80 mm Hg), apply second HemaShock® to the other leg.
In patients who have uncontrolled bleeding (e.g. intra-abdominal hemorrhage), the systolic blood pressure should be kept between 80 to 100 mm Hg, or as instructed by a physician (see Blood Pressure Titration by the HemaShock® paragraph below).
In other types of shock, the systolic blood pressure may be allowed to exceed 100 mm Hg.
Using the HemaShock® Flow Diagrams

Blood Pressure Titration by HemaShock®
- Rolling the HemaShock® up a limb increases blood pressure.
- Rolling it down will reduce systolic blood pressure.
Rolling is done by manually rolling the ring down the limb (picture). It should be done in small steps of about 15 cm (6″) each.
After each step, the blood pressure of the patient should be measured. If blood pressure falls to below 80 mm Hg, or other symptoms of hemodynamic instability (e.g. excessive tachycardia, cognitive deficit) is seen, consider bringing the HemaShock® back up. This should be done by pulling the straps as in the first application of the device.

Marking Placement Time & Removal Time
HemaShock® should not be left on a limb for more than 120 minutes (two hours).
In order to verify, it is important to mark the time of applying the HemaShock® on each limb very clearly using adhesive tape or stickers (picture).